Read the latest and greatest from our team
of incredible specialists.

Beach House Recovery Center » Blog » Guide to MAT Programs for Opiate Addiction
Medication-assisted treatment (MAT) is “the use of medications in combination with counseling and behavioral therapies for the treatment of substance use disorders,” according to the Substance Abuse and Mental Health Services Administration (SAMHSA). As such, MAT is a comprehensive treatment approach to the problem of cravings that describe addiction: any MAT should be administered in conjunction with counseling and behavioral therapy.
It is also worth emphasizing in relation to MAT that there is more than one medication option.
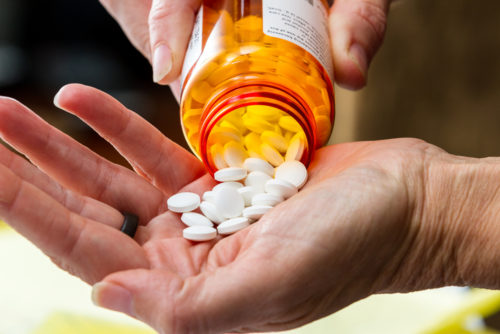
In recent years, in response to an escalating U.S. opiate epidemic, MAT programs have shown promise at treating opiate addiction, helping many people achieve recovery— despite the fact that less than half of privately funded treatment programs reportedly provide MAT and only one-third of clients receive the intervention. Findings cited by the National Institute on Drug Abuse (NIDA) have also revealed that MAT:
This guide to MAT programs for opiate addiction is therefore intended as a source of hope for anyone struggling with opiate addiction. You need to know that recovery is possible and that there is help, thanks to the best that medical and clinical experts have to offer.
A number of medications are now available to treat opiate addiction, having been found in clinical studies to reduce cravings and ease withdrawal symptoms, thereby lowering the risks of relapse. They include the following medications:
Buprenorphine is a “partial agonist” drug, meaning that it binds to the same opioid receptors that heroin and prescription painkillers do— only faster (effectively blocking these other “full agonist” drugs from working) and without the same euphoria. In essence, buprenorphine stops withdrawal in its tracks, but without unleashing the same addictive cycle of cravings followed by drug seeking. One drawback of buprenorphine is that it technically is still an opioid drug, and therefore can be addictive.
In rehab programs that administer MAT, clients should receive a complete physical exam and in-depth psychiatric assessment upon intake. The goal of the assessment is to determine whether they meet the criteria for opiate dependence—and therefore are candidates for MAT—and whether there are any other underlying physical and/or psychiatric issues at play. Clients may be asked questions like:
Clients will then be evaluated as to whether they formally meet the DSM-V criteria for opiate abuse and/or dependence. (The DSM-V is the handbook that clinicians use for diagnosing substance use and other mental disorders.)
Once an assessment has determined that a client is opiate-dependent, they, in close consultation with their attending psychiatrist, may then receive a MAT treatment plan. (Getting the green light to start a MAT will depend on whether there are other opiate or benzodiazepine drugs in the system, among other issues.) Any MAT treatment plan will be highly individualized and tailored to meet the personalized needs of the client. For example, if a client has a dual diagnosis—a co-occurring disorder such as bipolar disorder—this may require immediate medical attention at the start of treatment, thus delaying when MAT can begin.
The general guidelines for MAT published by SAMHSA recommend the introduction of a MAT during detox, as a way to help clients better weather the cravings and withdrawal symptoms that comprise the acute phase of treatment. The goal in this first phase of treatment is to use MAT to help clients get stabilized, so that they can better participate in the next “rehabilitative” phase of their treatment, consisting of group and individual behavioral therapies for opiate addiction.
During this rehabilitative period of treatment, which may run from only a few weeks to two to three months or longer, clients may taper off the MAT or they may continue with medication maintenance— depending on their treatment plan and the MAT they were prescribed. For example, while sometimes clonidine is prescribed for a longer period, the drug usually is taken for no more than 10 days (covering the acute phase of treatment that comprises detox and withdrawal); and, while studies have not identified one optimal window of time during which buprenorphine should be taken, research has revealed that longer-term maintenance of the drug is associated with better recovery outcomes. (There are also risks to taking Suboxone for too long, which are worth considering.)
By the time clients reach the rehabilitative phase of treatment, then, they may either be stabilized on the right MAT dose or will be tapering/will have tapered. During this rehabilitative phase, the goal is to learn healthy coping skills for dealing with the various life stressors that may have contributed to opiate abuse and dependency. Individual and group therapies, including peer support services, help clients develop these critical recovery tools that will help them sustain a life free of opiates in the long haul. Depending on their plan of treatment, a MAT may or may not belong to their longer-term, post-rehab arsenal of coping tools.
36 percent of the more than five million Americans who were taking opiates for non-medical reasons in 2016 met the diagnostic criteria for opiate abuse and dependence, according to a 2016 article in the Open Journal of Psychiatry. Thanks to cutting-edge research that is advancing every day, MATs in combination with therapies are helping many people in their same shoes recover from their addiction. Not only that, research is well underway into new MATs that might be added to the above list— with promising results. In the meantime, knowing there are options when it comes to MAT is one more reason to believe there is life after opiate addiction.
For more information related to MAT and opiate addiction, see the following articles:
Whether you’re researching for yourself or a loved one, Beach House can help. We understand that this is a serious time in your life and that the treatment center you choose matters. We want you to feel comfortable and empowered to make the right decision for yourself, a friend, or a family member. This is why a counselor is waiting and available to answer your questions and help put your mind at ease regarding the next steps. Many of the staff at Beach House have walked in your shoes. If you feel you’re ready or want more information about how to help a loved one, we can help today. You can also learn why we are voted the #1 rehab for addiction treatment in Florida.
We accept most major insurance plans and can verify your benefits quickly and confidentially.
We’re committed to helping you access the care you need, our admissions counselors can guide you through your coverage options and available resources.





"*" indicates required fields