Read the latest and greatest from our team
of incredible specialists.

Beach House Recovery Center » Blog » Effects of Snorting Adderall
Adderall is a prescription stimulant that is increasingly abused by those seeking enhanced energy levels and sharpened mental focus. Adderall is also prized for the euphoria it induces when taken in high doses—especially through improper methods such as snorting, smoking, or intravenous (IV) injection. Among adolescents, snorting is considered the second most common method of ingestion, and by far the most dangerous. Adderall is considered a Schedule 11 Substance by the Drug Enforcement Administration (DEA)—a designation reserved for substances with a high potential for addiction and abuse. Although the drug continues to be legitimately prescribed to treat attention deficit hyperactivity disorder (ADHD) and narcolepsy, its epidemic-level diversion and abuse have overshadowed its short-term benefits.
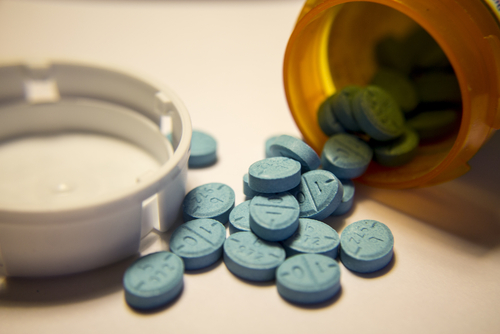
The prevalence of Adderall abuse amongst college students—many who abuse the drug exclusively through snorting—has surged in recent years due to using the drug as a study aid. The following statistics underscore the dangers associated with the drug:
Snorting is a quick-delivery method of ingestion in which the powdered form of the drug is inhaled through the nasal cavities into the nasal membranes and delivered to the bloodstream by the surrounding blood vessels. The blood vessels, in turn, deliver it to the heart where it is pumped to the brain and the rest of the body. Snorting produces a more immediate, intense high making it a popular vehicle for recreational abuse.
Snorting Adderall is usually accomplished by removing the medication from the capsule and grinding it up into a fine powder, then splitting it into lines. At this point, the user utilizes a straw or rolled piece of paper to inhale the crushed powder through the nose. The moist mucous membranes making up the nasal tissues pass the drug into the network of surrounding blood vessels. This process takes approximately 5-10 minutes for the Adderall to be fully absorbed and penetrate the blood-brain barrier so that the Adderall “high” can be experienced.
People who snort Adderall usually take much more of the drug than those who ingest it orally, making them prone to quickly developing a tolerance for and, ultimately, dependency on the drug. Snorting can not only damage the delicate membranes inside the nose and sinuses, but also those of the respiratory system making the user more susceptible to airborne infections and diseases. Snorting has also been known to lead to high fevers, toxic shock, and sudden death.
Of particular concern are the potential psychotic effects of Adderall abuse, whereby a user might experience auditory or visual hallucinations, as well as become totally out-of-touch with reality. They may also exhibit sudden violent reactions or become severely agitated for no apparent reason. Initially, a user may feel extremely productive and intelligent, but they frequently experience a total emotional and physical crash as the drug wears off. Lack of sleep and hyperactivity eventually catches up with the user, causing difficulty concentrating at work or school, and a subsequent loss of productivity.
Adderall was originally considered a ‘smart drug’ due to its reputation for improving academic performance, a myth that has been shattered by emerging data. In addition to the deleterious effect the drug has on grade point averages (GPAs), it produces a number of dangerous physical and psychological side effects including:
Snorting or huffing is one of the primary causes of a drug overdose, and those who irresponsibly use this practice of drug delivery are frequently evasive and extremely adept at hiding their habit from others. However, there are certain signs that can be used to help determine whether a loved one is snorting Adderall. They include:
A combination of any of these signs or symptoms should set off an alarm that a loved one needs help. Any sudden or extremely severe symptoms require immediate first aid which should include putting the person in a bathtub filled with ice water to bring the temperature down quickly. As a first step, try to ascertain the amount of Adderall that was ingested in order to better help medical personnel, and arrest dehydration by providing plenty of fluids.
Ingesting high doses of Adderall can raise a user’s blood pressure as well as heart rate to extremely dangerous levels, leading to seizures, heart failure, and possible death. Because of the binge-oriented nature of Adderall abuse, accidental overdose is a likely scenario. The Substance abuse and Health Services Administration (SAMHASA) states that there is an increasing pattern of Adderall—or methamphetamine—abuse among young adults, with over 31,000 emergency room (ER) visits annually. The following are common signs of Adderall overdose:
There are also several factors that can put a user at a greater risk of an Adderall overdose. These include:
Only trained medical professionals and licensed clinicians possess the education, hands-on training, and acquired skill set necessary to treat Adderall addiction—especially when it is the result of improper ingestion by snorting. The following stages of treatment form the basis of professional intervention and lead to the most favorable long-term recovery outcomes
Addiction is not a disease affecting only those with known substance use disorders (SUDs) or genetic susceptibility. Anyone, at any time, regardless of race, gender, socioeconomic status, age, or religion can find themselves addicted to Adderall and in need of professional treatment. If you or someone you love is addicted to Adderall and in need of help, call a substance abuse addiction treatment professional today.
And remember, in the event of an Adderall overdose, immediately call 911 or visit your nearest hospital emergency room (ER).
For more about Adderall addiction and recovery, check out these related articles:
Sources:
Johns Hopkins University— Hub Staff Report. Adderall abuse on the rise among young adults. Feb, 2016.
Brain and Behavior. Prescription stimulants in individuals with and without attention deficit hyperactivity disorder: misuse, cognitive impact, and adverse effects. September 2012.
Journal of the American Academy of Child and Adolescent Psychiatry. Adderall and the FDA. Vol 40, 2001.
Pharmacy. Neurocognitive, Autonomic, and Mood Effects of Adderall: A Pilot Study of Healthy College Students. September, 2018.
ASPET Pharmacological Reviews. Psychostimulants and Cognition: A Continuum of Behavioral and Cognitive Action. Jan, 2014.
Whether you’re researching for yourself or a loved one, Beach House can help. We understand that this is a serious time in your life and that the treatment center you choose matters. We want you to feel comfortable and empowered to make the right decision for yourself, a friend, or a family member. This is why a counselor is waiting and available to answer your questions and help put your mind at ease regarding the next steps. Many of the staff at Beach House have walked in your shoes. If you feel you’re ready or want more information about how to help a loved one, we can help today. You can also learn why we are voted the #1 rehab for addiction treatment in Florida.
We accept most major insurance plans and can verify your benefits quickly and confidentially.
We’re committed to helping you access the care you need, our admissions counselors can guide you through your coverage options and available resources.





"*" indicates required fields