TABLE OF CONTENTS
When casual drinking progresses to everyday use, or when drinking and drug use coincide, addiction may soon follow. The chronic drinker experiences negative consequences and serious repercussions more often, until functioning normally is impossible. Job loss, family dysfunction, relationship issues, financial troubles and legal woes may finally convince the alcoholic to accept treatment. Or, the family stages a formal intervention to encourage the addict to get professional help.
The first step in the process of recovery from alcohol abuse or addiction is a safe, medically supervised detox, which eliminates alcohol from the body so that the client can proceed to the next level of alcohol treatment. What follows is a detailed introduction to alcohol detox, starting with common withdrawal symptoms and a timeline for early recovery.
Is alcohol ruining your life? Call: (855) 935-2871
ALCOHOL WITHDRAWAL SYMPTOMS
 Among patients with alcohol dependence, approximately 50 percent experience alcohol withdrawal. The New England Journal of Medicine reports that 3-5 percent of those with AUDs experiencing alcohol withdrawal will suffer seizures or severe delirium when discontinuing alcohol use.
Among patients with alcohol dependence, approximately 50 percent experience alcohol withdrawal. The New England Journal of Medicine reports that 3-5 percent of those with AUDs experiencing alcohol withdrawal will suffer seizures or severe delirium when discontinuing alcohol use.
Alcohol withdrawal symptoms, part of alcohol withdrawal syndrome, range from mild to severe, with the most consequential symptoms occurring in patients with severe complicated alcohol withdrawal.
The Clinical Institute Assessment of Alcohol Withdrawal Scale lists nine items for assessing symptoms and severity of alcohol withdrawal. These are scored on a scale ranging from 0 to 7 (the most severe):
- Agitation – with most severely affected patients pacing during assessment.
- Anxiety – most severe form is acute panic.
- Headache – high end of scale is extremely severe headache.
- Nausea or vomiting – patient with most severe symptoms have continuous nausea and vomiting.
- Paroxysmal sweats – in most severely affected patients, the symptom is drenching sweats.
- Tactile, auditory and visual disturbances – most severe form is continuous hallucinations.
- Tremor – at the high end of the scale, patients exhibit severe tremor.
Treatment professionals will monitor the patient undergoing alcohol withdrawal and prescribe medications or therapies to help ease the discomfort and reduce the severity, length and frequency of the various withdrawal symptoms the patient experiences.
How lengthy or severe withdrawal symptoms are can depend on many factors. Those who have chronically abused alcohol will likely take longer to fully detox and may experience more severe alcohol withdrawal symptoms, possibly even alcohol withdrawal syndrome. Among those diagnosed with alcohol addiction and addiction to other drugs, withdrawal symptoms may also be protracted, require careful pharmacological intervention and/or other forms of therapy to ease detox. Family history of alcoholism plays a factor as well as genetic predisposition to alcohol abuse.
Alcohol withdrawal symptoms can be brief, lasting 1-2 days, or persist for more than a week. Some symptoms may continue long after initial alcohol detox, particularly brain-related changes caused by alcohol addiction, such as confusion, memory loss, difficulty with focus and concentration.
ALCOHOL WITHDRAWAL TIMELINE
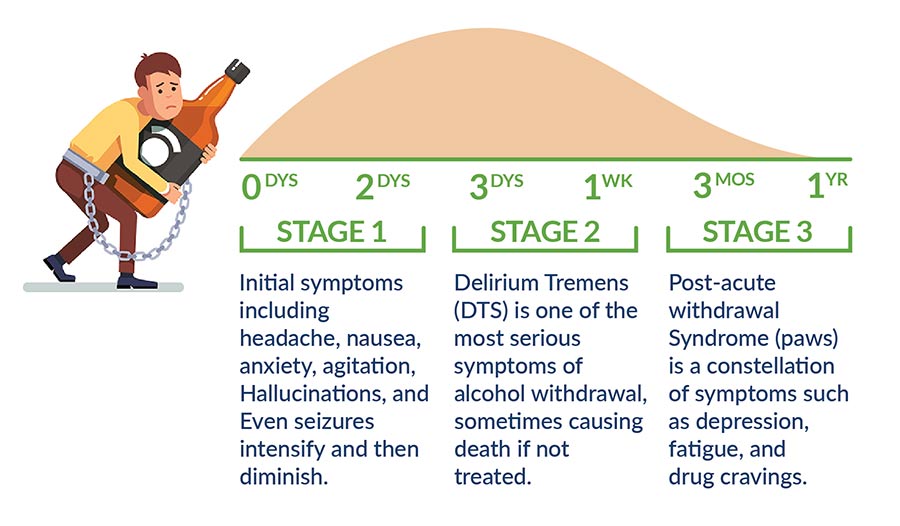
Initial alcohol withdrawal symptoms typically appear between 6 and 48 hours after cessation of heavy or excessive alcohol consumption. Initial symptoms of headache, sweating, agitation, anxiety, irritability, nausea and vomiting, sensitivity to light and sound, tremors, disorientation and difficulty concentrating intensify first and then diminish over 24-48 hours.
Hallucinations, a major alcohol withdrawal symptom, occurs 10-72 hours after the last drink.
Seizures, a more serious alcohol withdrawal symptom, usually begin within 24 hours after quitting drinking. Seizures don’t happen to everyone, occurring in about 25 percent of those undergoing alcohol withdrawal. They are generally brief: About 60 percent of patients experience them as multiple short seizures. Seizures may also result from combined alcohol and stimulant use (cocaine or amphetamines), or when withdrawing from alcohol and sedatives (barbiturates or benzodiazepines).
Delirium tremens (DTs) – Delirium, one of the most serious symptoms of alcohol withdrawal, generally occurs about three days after first appearance of alcohol withdrawal symptoms. It lasts anywhere from 1-8 days or more, although typically, the duration is 2-3 days. Delirium during alcohol withdrawal can be predicted by the presence of high blood pressure, older age, prior episodes of seizures or delirium, recent use of depressants, and concomitant medical disorders. Approximately 1-4 percent of hospitalized patients with DTs die. Death is usually the result of hyperthermia, concomitant medical conditions, heart problems, or complications from seizures. Earlier diagnosis and treatment with intravenous benzodiazepines or other sedative therapy can potentially reduce number of deaths.
Post-acute withdrawal syndrome (PAWS) is not part of alcohol detox, but generally occurs after the cessation of alcohol use. PAWS is a constellation of symptoms, primarily psychological (mood swings, depression, cognitive impairment, depression, anxiety, fatigue, sleep patterns, stress response, drug cravings), that last for several months or even up to a year or longer.
How long does alcohol stay in your body? Alcohol is quickly absorbed by the body, although it takes much longer to leave. Alcohol gets to the stomach via the bloodstream in the first 5 minutes. About 20 percent of it stays there and 80 percent goes to the small intestine, pancreas and then to the liver, where it is metabolized. Alcohol is metabolized at a rate of 0.015 of blood alcohol content (BAC) per hour. Alcohol stays in the blood for 12 hours, 5 days in urine, and up to 90 days in hair.
INPATIENT TREATMENT FOR ALCOHOL
 Inpatient treatment is not technically detox, which is a separate level of care that precedes inpatient treatment. After admission to the inpatient treatment facility, the client goes through medically-managed detox first and then progresses to the formal treatment program, consisting of clinical and medical therapies targeting his or her addiction and specific needs and recovery goals.
Inpatient treatment is not technically detox, which is a separate level of care that precedes inpatient treatment. After admission to the inpatient treatment facility, the client goes through medically-managed detox first and then progresses to the formal treatment program, consisting of clinical and medical therapies targeting his or her addiction and specific needs and recovery goals.
During a client’s residence in a rehab facility, they may receive treatments that include one-on-one counseling, group counseling, and behavioral therapy, including cognitive behavioral therapy (CBT), dialectical behavioral therapy (DBT), motivational interviewing (MI), medication-assisted treatment (MAT), mindfulness meditation, yoga, family therapy, and peer support and life-skills group.
Medication-Assisted Treatment
Clients may also receive Medication-Assisted Treatment (MAT) to relieve alcohol cravings and assist in the adjustment to sobriety. There are currently three FDA-approved drugs to treat alcohol withdrawal: naltrexone, acamprosate, and disulfiram:
- Naltrexone is effective in treating alcohol dependence, resulting in decreases in the length and frequency of drinking bouts and avoid relapses, although the medication has severe side effects that are difficult to overcome. A study published in Alcoholism, Clinical and Experimental Research found that, in nicotine-users/smokers diagnosed with AUD, naltrexone was effective in significantly reducing percent heavy drinking days (PHDD). Naltrexone is not addictive, does not interact negatively with alcohol, and is most effective when used in long-term therapy extending beyond three months (even indefinitely).
- Acamprosate is a medication in tablet form for treatment in recovery from AUD who have stopped drinking. It is typically given on the 5th day of abstinence and achieves full effectiveness in 5-8 days. Acamprosate prevents drinking but does not prevent withdrawal symptoms after drinking. The medication has not been shown to work in those who continue drinking, use illicit drugs, and/or prescription drug abuse/misuse.
- Disulfiram is a once-daily tablet medication for chronic alcoholism and is most effective in those who have already gone through detox or are in the early stage of abstinence. It should not be taken when intoxicated or for 12 hours after drinking.
None of the three drugs for AUD is a cure on its own and are most effective when part of a medication-assisted treatment (MAT) program. MAT consists of medication, counseling and behavior therapies to treat SUDs, including AUDs.
The gold standard for treatment of alcohol withdrawal has long been the use of benzodiazepines, for which there is a larger evidence base. Yet, frequent use of benzodiazepines causes cross-tolerance, dependence and cross-addiction to alcohol. Diazepam, according to research on the treatment of severe alcohol withdrawal, has the most favorable pharmacokinetic profile, and the use of protocolized benzodiazepine escalation may be more effective than symptom-triggered medication usage, while also possibly decreasing the need for ventilation and lengthier stays in the intensive care unit (ICU).
A review of literature shows that propofol may be a good alternative to benzos, although more study on the roles of ketamine, phenobarbital and dexmedetomidine is needed. Some research points to the effectiveness of dexmedetomidine as an adjunct to benzodiazepine therapy alone in treating severe symptoms of delirium.
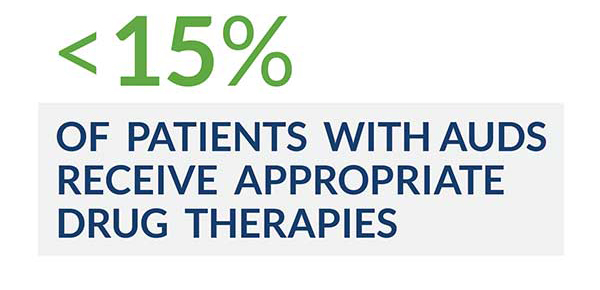 Due to the presence of comorbidities, concomitant use of more than one medication, and the interference of alcohol, alcoholics are at high risk of drug-to-drug interactions. As such, according to research, many physicians are reluctant to prescribe the appropriate pharmacological medications. As a result, less than 15 percent of patients with the most severe AUDs receive appropriate drug therapies.
Due to the presence of comorbidities, concomitant use of more than one medication, and the interference of alcohol, alcoholics are at high risk of drug-to-drug interactions. As such, according to research, many physicians are reluctant to prescribe the appropriate pharmacological medications. As a result, less than 15 percent of patients with the most severe AUDs receive appropriate drug therapies.
Medications used to treat anxiety disorders may include selective serotonin reuptake inhibitors (SSRIs), although they may cause an increase in drinking in those who are actively drinking. For those with co-occurring anxiety disorder and AUD, gabapentin, pregabalin and buspirone were found to be effective in one review of the literature.
On the horizon for alcohol addiction treatment, University of Rhode Island researchers have discovered what they term “promising” therapy for alcohol abuse and are targeting a federally funded larger clinical trial of a drug focusing on blocking ghrelin, the “hunger hormone.” Preliminary results from the initial clinical trial of the medication showed significant reduction in alcohol and food cravings, the drug was safe and well tolerated, and did not affect alcohol pharmacokinetics.
The National Institute on Alcohol Abuse and Alcoholism (NIAAA) notes that its current research shows promise for other medications in treating alcohol dependence and problem drinking:
- Varenicline (marketed as Chantix), the anti-smoking drug has shown reduced alcohol consumption/craving in clinical tests in alcoholics.
- Topiramate, the anti-epileptic drug, shows effectiveness in helping problem drinkers, especially those with a particular genetic makeup, curb alcohol use.
- Gabapentin, a drug prescribed to treat epilepsy and pain, showed reduced heavy drinking, fewer alcohol cravings, better mood and sleep, and longer alcohol abstinence.
Dual diagnosis treatment
Patients diagnosed with AUD and co-occurring mental health disorder, called “dual diagnosis,” should receive concurrent treatment for both. It is also noteworthy that studies have found that those with a history of a mental disorder are more likely to develop a lifetime AUD. During detox from alcohol, medications to ease the length, frequency and severity of symptoms as well as medication prescribed to help with mental health disorders, including anxiety, depression, bipolar disorder, post-traumatic stress disorder (PTSD) and others may be used. During formal phase of treatment, appropriate pharmacological treatments may continue to be used in the management of ongoing or persistent alcohol withdrawal symptoms and treating the existing mental health disorder.
In addition to any medications prescribed, the patient enrolled in inpatient or residential treatment for alcohol addiction will receive a number of treatment modalities, including individual counseling, targeted behavioral and alternative therapies, group counseling sessions, educational lectures, training in relaxation techniques, leisure activities, skills-based training, introduction to 12-Step groups and more.
Learn more about our Alcohol Detox Program
OUTPATIENT TREATMENT FOR ALCOHOL
Outpatient treatment may be provided at stand-alone outpatient facilities, in hospitals, clinics and doctor’s offices. As the name implies, the client goes to the facility for treatment and then returns home, coming back for or being referred to outpatient alcohol addiction treatment facilities for ongoing medication/therapies and counseling as appropriate.
Outpatient services for alcohol can include medical and clinical interventions that ideally are tailored to meet clients’ individualized treatment needs. (To learn more about these various treatment options, please see the above section on Inpatient Treatment.)
Learn more about Outpatient Alcohol Rehab
CAN ALCOHOL DETOX BE DONE AT HOME?
While the temptation to go it alone and detox from alcohol at home may spring to mind as easier, quicker and less expensive, this is never a good idea. For one thing, there’s no medical professional available 24/7 to monitor your detox progress, the presence, frequency, length and severity of withdrawal symptoms, or the emergence of potentially life-threatening complications, such as seizures, cardiac arrest, or delirium, to name a few. Furthermore, once you begin to experience withdrawal symptoms, and the more uncomfortable or painful they become, you’re likely to give up and go back to using alcohol. This defeats the purpose of detox and puts you right back where you started— addicted to alcohol.
On the other hand, a skilled and certified medical professional can help you detox safely and effectively. You’ll experience minimal or greatly reduced withdrawal symptoms and come through detox ready to begin addressing alcohol addiction through comprehensive, integrated alcohol addiction treatment.
TAPERED VS. COLD TURKEY
A big issue when considering detox for alcohol addiction is whether it is safe. When alcohol detox is administered under medically monitored conditions by alcohol addiction detox professionals, it is very safe. The decision to do a tapered or stepped-down dose or cold turkey, abruptly stopping alcohol, is one made by the treating professionals. There is, however, no gradual cessation of alcohol use in medical alcohol detox. Heavy or problem drinkers may first try to gradually cut down on alcohol consumption before attempting to quit drinking. This may or may not be successful. In medically-monitored alcohol detox, medications are often used, as appropriate, to help lessen the severity, duration and frequency of unpleasant alcohol withdrawal symptoms. Best practices favor using such medications in a symptom-triggered regime instead of a fixed-dose tapering schedule. Severe alcoholism detox is a serious procedure that entails some risk of complications and can be life threatening if the alcoholic attempts to go cold turkey on his or her own.
Trying to quit drinking on your own may seem like a quick and easy solution to problem drinking, and it is the least expensive option. Yet, the fact that there’s no medical help available to manage the number, frequency and severity of alcohol withdrawal symptoms and/or medical complications should be strongly considered. In addition, when you go it alone, you’re much more likely to give up and resume drinking just to stop unpleasant or painful withdrawal symptoms. There is a threshold of tolerance to such symptoms that may tip you over the edge. The longer you’ve been a heavy drinker, the more difficult it will be to quit on your own. Professional detox is a safer and more effective choice.
CONSIDERATIONS/HOW TO DECIDE WHAT IS RIGHT FOR YOU
Location may be one factor to consider when deciding on where to go to receive treatment. Some patients favor being close to home and family, while others choose a treatment facility far away from home, so they’re completely separated from the people, places and things associated with their alcohol use. While each has its pros and cons, careful weighing of what makes sense for you will likely help you make the right choice.
Insurance coverage is another important consideration in choosing where, when and how to get treatment for alcohol addiction. Depending on your insurance coverage, some or most of your substance abuse treatment may be covered.
Private treatment is an option that may be preferred, due to the high staff-to-client ratio, availability of an array of treatment modalities and specialized treatments, the treatment facility’s success rate treating alcoholism and/or other substances and mental health disorders, reputation, amenities, leisure activities, detox on-site, aftercare and alumni services and other components of a comprehensive, integrated addiction treatment program.
Without question, outpatient treatment is the least costly option for alcohol detox and treatment. For those who want or require inpatient or residential alcohol addiction treatment, either 30-day or long-term treatment (three to six months or longer), expect to pay considerably more. The effectiveness of treatment outcome, however, may be more skewed toward residential treatment, in terms of reductions in risk of relapse. If you’ve repeatedly relapsed or have dual diagnosis, residential treatment may be the recommended choice.
Most of the best treatment facilities offer payment plans for those whose insurance does not cover or fully cover treatment. Some offer scholarships, while others can refer patients to treatment centers or facilities or to federal, state and local agencies to receive financial assistance, grants and other forms of aid.
RECOVERY SUCCESS AND AFTERCARE SERVICES FOR ALCOHOL
Success rates for recovery improve the longer the patient remains in treatment. Following completion of formal treatment, then, aftercare services are strongly encouraged. Besides the strong recommendation, backed by research, for recovering alcoholics to attend 12-Step groups such as AA, additional services following treatment may be available. These are known as aftercare services, or continuing care services and are offered by the best alcohol and drug addiction treatment facilities.
Aftercare options can include:
- individual maintenance sessions with a skilled therapist
- medication management
- regular check-ins (including random drug tests)
- active alumni services
- life and wellness coaching
Continuing psychiatric counseling, group counseling, participating in 12-Step and other recovery groups, including peer recovery groups, staying up-to-date on prescribed medications, keeping all doctor appointments, tending to spiritual development, and learning and practicing healthier behaviors all contribute to long-term alcohol addiction recovery. And treatment outcomes are better among clients who continue with these commitments.
Learn more about Alcohol Aftercare
Is alcohol ruining your life? Get help now
Acta Pharmacologica Sinica. “Alcohol use disorders and current pharmacological therapies: the role of GABA(A) receptors.” August 2014.
Alcohol. “Changes in the serum metabolite profile correlate with decreased brain grey matter volume in moderate-to-heavy-drinking young adults.”
Alcoholism, Clinical and Experimental Research. “Nicotine-Use/Smoking Is Associated with the Efficacy of Naltrexone in the Treatment of Alcohol Dependence.” February 12, 2018.
Alcoholism, Clinical and Experimental Research. “The effects of age at drinking onset and stressful life events on alcohol use in adulthood: a replication and extension using a population-based twin sample.” June 2012.
Frontiers in Psychiatry. “Treatment of Comorbid Alcohol Dependence and Anxiety Disorder: Review of the Scientific Evidence and Recommendations for Treatment.” September 22, 2017.
JBI Database of Systematic Reviews and Implementation Reports. “The use of dexmedetomidine as an adjuvant to benzodiazepine-based therapy to decrease the severity of delirium in alcohol withdrawal in adult intensive care unit patients: a systematic review.” January 2015.
Journal of Clinical and Diagnostic Research. “Alcohol Withdrawal Syndrome: Benzodiazepines and Beyond.” September 1, 2015.
Journal of Substance Abuse Treatment. “Barriers and facilitators to successful transition from long-term residential substance abuse treatment.” March 2017.
National Council on Alcoholism and Drug Dependence, Inc. “Am I An Alcoholic Self Test.”
National Institute on Alcohol Abuse and Alcoholism. “Treatment for Alcohol Problems: Finding and Getting Help.” 2014.
New England Journal of Medicine. “Recognition and Management of Delirium (Delirium Tremens).” November 27, 2014.
Pharmacological Research. “Drug-drug interactions in the treatment for alcohol use disorders: A comprehensive review.” April 30, 2018.
Revista de Psichiatria. “Pharmacological treatment for dual diagnosis: a literature update and a proposal for intervention.” May-June 2018.
SAMHSA. “Key Substance Use and Mental Health Indicators in the United States: Results from the 2016 National Survey on Drug Use and Health.” September 2017.
SAMHSA’s National Registry of Evidence-Based Programs and Practices. “Alcohol Behavioral Couple Therapy.” January 2009.
Substance Abuse and Mental Health Services Administration (SAMHSA). “Medication and Counseling Treatment.”
The Annals of Pharmacotherapy. “Treatment of Severe Alcohol Withdrawal.” May 2016.
University of Rhode Island. “URI drug study produces ‘promising therapy’ for alcohol abuse.” June 28, 2018.
Related Articles:
How Long Does it Take to Detox From Alcohol







