Xanax Detox – Withdrawal Symptoms and Timeline
[three-fifths-first]
Xanax, a benzodiazepine medication introduced in 1981, is used to treat anxiety and panic disorders. In the early twenty-first century, it was the most commonly prescribed psychotropic (mood-altering) drug in the United States. Xanax is normally sold as “immediate-release” tablets to take in case of anxiety attack, or as daily-dose “extended-release” tablets.
Like other benzodiazepines, Xanax is a tranquilizer that inhibits muscle-tremor and panic reflexes. Because physical dependence can develop within four to six weeks, it is best used as a short-term solution so patients can regain normal functioning long enough to learn non-drug coping strategies. Unfortunately, the “quick fix” tempts many people to keep relying on the drug. Regular users range from senior citizens to middle school students. They also include executives and popular entertainers: it’s not uncommon to hear Xanax extolled in rap lyrics.
[/three-fifths-first]
[two-fifths]
TABLE OF CONTENTS
[/two-fifths][clearfix]
The demand for illicit Xanax is high enough that “counterfeit” pills are also sold widely. These contain no actual benzodiazepine and often substitute fentanyl, a super-potent and extremely dangerous opioid. Even with pharmacy-provided Xanax, some users increase their overdose risk by crushing extended-release tablets to extract larger doses.

Nearly 125,000 emergency-room visits a year are due to using Xanax apart from official medical instructions.
Is Xanax ruining your life? Call: (855) 935-2871
XANAX EFFECTS AND ADDICTION
However it’s used, Xanax quickly induces an overall sense of calm and sometimes euphoria. (Many people, however, report less desirable effects such as drowsiness, poor coordination and memory problems.) Under the influence of Xanax, muscles relax and heart rate slows. If enough is taken to induce an overdose (which requires immediate medical attention), common symptoms include:
- Sudden and severe drowsiness
- Mental confusion
- Lethargy
- Loss of physical coordination
Someone who develops addiction may become chronically drowsy and sluggish, or complain of blurred vision and dizzy spells. Some medical experts believe that long-term overuse can cause permanent brain damage.
XANAX WITHDRAWAL SYMPTOMS
If the Xanax supply is abruptly cut off, typical withdrawal symptoms include:
[one-half-first]
- Depression
- Insomnia
- Panic sensations
- Rising blood pressure
- Heavy perspiration
- Chills
[/one-half-first][one-half]
- Nausea and vomiting
- Stomach cramps
- Accelerating heart rate
- Convulsions
- Delirium
[/one-half][clearfix]
Seizures can also happen during withdrawal from Xanax— yet another reason why medically monitored detox is the only option for anyone with a Xanax dependency.
Withdrawal symptoms are likely to be most severe in people who have taken Xanax for long periods in heavy doses, have used other drugs or have additional physical or mental health conditions.
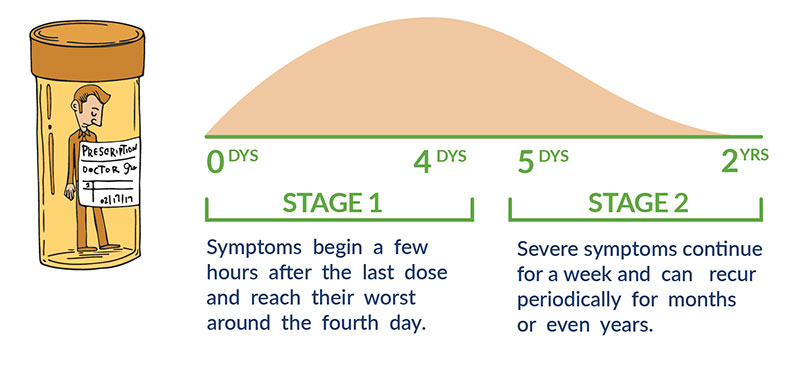
XANAX WITHDRAWAL TIMELINE
Xanax has among the shortest of drug half-lives, which means it leaves the body quickly but also manifests withdrawal symptoms quickly. When the drug is stopped cold turkey, symptoms begin a few hours after the last dose and reach their worst around the fourth day as the physical system flushes out the last of the actual Xanax. Severe symptoms continue for about a week as the body adjusts to the absence of its accustomed chemical crutch. However, symptoms can recur periodically for months or even years.
As with any addiction, relapse remains a high risk for some time, particularly when old stresses or drug-use associations resurface. This is one reason why professional treatment, with therapy, is always recommended for getting off Xanax. The best therapy covers:
- What caused the addiction. Are the patient’s anxiety issues rooted in trauma, perfectionism, low self-confidence? How did the original Xanax prescription get out of control?
- Physical health. Healthy energy levels—fueled by a healthy diet and regular physical activity—equip a person to better resist relapse.
- Self-esteem. Most people who develop addictions feel chronically unsure of themselves, unlikely to succeed in anything or even unworthy of anything good. These issues need to be dealt with to ensure motivation for long-term sobriety.
- Relapse prevention. Anyone with an addiction disorder needs a plan for avoiding “triggers” and a plan to recover quickly in the event of relapse (there’s no way to absolutely guarantee it won’t happen, but there are ways to keep it from ending back in full dependence).
INPATIENT TREATMENT FOR XANAX
When it comes to choosing a treatment program, the first big decision (aside from the center’s reputation and qualifications) is usually whether to register for inpatient or outpatient treatment. With inpatient care, the patient lives in detox-center-supervised housing throughout several weeks or months of post-detox rehab. Inpatient care is recommended if:
- The patient is likely to encounter relapse triggers shortly after release.
- The patient lacks a strong support network outside the treatment center.
- The patient has co-occurring mental health disorders.
Few patients fresh from detox are ready to resist old temptations immediately. In inpatient care, temptations are guaranteed to remain a safe distance away, and professional support near at hand. Other advantages of inpatient care include:
- More opportunities to meet peers with similar struggles and realize others have been there too
- Assurance of adequate nutrition at every meal
- Hands-on opportunities to discover new interests at the center’s recreational facilities
OUTPATIENT TREATMENT FOR XANAX
With outpatient care, a patient lives offsite and reports to detox facilities for ongoing therapy.
Outpatient care may be preferable for someone who:
- Has remained functional in outside responsibilities
- Can easily arrange his or her schedule to minimize risk of encountering relapse triggers
- Has supportive family and friends to help keep things on track
- Can live in a location convenient to the treatment center
Some detox centers use a combination approach—at least 30 days of inpatient treatment followed by 30-60 days of outpatient care.
CAN XANAX DETOX BE DONE AT HOME?
Regardless of what program is chosen for post-detox rehab, physical detox should always be undertaken in an inpatient setting, especially with benzodiazepines and especially with short-acting benzos such as Xanax. Physical withdrawal from Xanax and other benzo drugs comes with high risk of potentially life-threatening reactions:
- Heart palpitations
- Difficulty breathing
- Seizures
- Panic or hallucinations that may trigger dangerous actions
Besides staff experienced in nursing care and emergency first aid, detox centers have access to licensed MDs who can arrange for prescription medications if these are needed to ease withdrawal.
TAPERED VS. COLD TURKEY
Benzodiazepine detox providers frequently use the “tapered” approach, administering gradually reduced doses rather than abruptly cutting off the supply. “Tapering” spares the body and brain the worst of cold-turkey shock. Often a benzodiazepine with a longer half-life (Klonopin, Librium and Valium are popular options) is substituted for Xanax, to reduce the risk of complications by allowing for less frequent doses.
Perhaps the biggest risk of tapering is that a patient will become impatient. Getting completely “clean” of benzos can take a year or more, and consequences could be lethal if someone yields to temptation to either quit abruptly or give up and return to the old dose. Anyone on a tapering program should make sure they have ongoing therapy and support.
CONSIDERATIONS/HOW TO DECIDE WHAT IS RIGHT FOR YOU
Other factors to consider in choosing a treatment program include:
- Location (geographically convenient is usually best)
- Philosophical or religious emphasis
- Experience treating Xanax/benzodiazepine addiction in particular
Cost—and what health insurance/VA/Medicare will pay for—is another consideration. However, even the most expensive treatment option may spare a heavy Xanax user years of additional costs for Xanax, related health issues and lost productivity. If insurance doesn’t cover everything, payment plans, charitable assistance and outpatient options can reduce financial strain.
RECOVERY SUCCESS AND AFTERCARE SERVICES FOR XANAX
Even after official treatment is complete, recovery is a lifelong journey—the specter of relapse temptations rarely is completely exorcised. The best way to minimize risks of relapse is to stay in close touch with a support network: regular participation in a 12-Step or similar group can cut the danger by as much as half.

- Continued therapy for addiction-related issues
- Aftercare programs, including “alumni events,” at the detox center
- Volunteer work
- Religious involvement
- Developing new, healthy interests
[clearfix]
Is Xanax ruining your life? Get help now
[expand title=" Sources:" targclass="highlight"]
Bean, Shawn (2016, June 8). “Xanax ‘Helps Me Be a Better Mom.’” CNN.com. Retrieved from https://www.cnn.com/2013/02/18/health/parents-antidepressants/index.html
Blaszczak-Boxe, Agata (2016, February 22). “Overdoses on Anti-Anxiety Meds Such as Valium and Xanax Are on the Rise.” The Washington Post. Retrieved from https://www.washingtonpost.com/national/health-science/overdoses-on-anti-anxiety-meds-such-valium-and-xanax-are-on-the-rise/2016/02/22/4f6a6d8e-d727-11e5-be55-2cc3c1e4b76b_story.html?utm_term=.1a72c2879664
Chan, Stella (2017, June 6). “11 Middle Schoolers Hospitalized After Sharing Xanax.” CNN.com. Retrieved from https://www.cnn.com/2017/06/06/health/children-hospitalized-xanax-trnd/index.html
CNN.com (2014, May 22). “Xanax-Related ER Visits Double in 6 Years.” Retrieved from http://thechart.blogs.cnn.com/2014/05/22/xanax-related-er-visits-double-in-6-years/
Ganim, Sara (2017, March 17). “Pill Presses for Counterfeit Drugs Seized in Record Numbers.” CNN.com. Retrieved from https://www.cnn.com/2017/03/17/health/pill-presses-counterfeit-fentanyl/index.html
Johnson, Brian, and Jon Streltzer (2013, August 15). “Risks Associated with Long-Term Benzodiazepine Use.” American Family Physician, Vol. 88, No. 4, pp. 224–225. Retrieved from https://www.aafp.org/afp/2013/0815/p224.html
Jordan, Jay R. (2018, March 22). “Houstonians Arrested with Enough Fentanyl to ‘Kill Everyone in Toledo.’” Houston Chronicle. Retrieved from https://www.chron.com/news/houston-texas/houston/article/fentanyl-arrest-Houston-Ohio-enough-to-kill-12775134.php
National Institute on Drug Abuse (2018, July). “Commonly Abused Drugs Charts: Central Nervous System Depressants.” Retrieved from https://www.drugabuse.gov/drugs-abuse/commonly-abused-drugs-charts#CNSdepressants
National Institute on Drug Abuse (2011, May). “Drug-Related Hospital Emergency Room Visits.” Retrieved from https://www.drugabuse.gov/publications/drugfacts/drug-related-hospital-emergency-room-visits
National Institute on Drug Abuse (2017, September). “Overdose Death Rates.” Retrieved from https://www.drugabuse.gov/related-topics/trends-statistics/overdose-death-rates
Olsen, Lise (2010, December 13). “Abuse of Prescription Drugs Is on the Rise Across Texas.” Houston Chronicle. Retrieved from https://www.chron.com/news/houston-texas/article/Abuse-of-prescription-drugs-is-on-the-rise-across-1697224.php
O’Neill, Julie (2012, April 30). “Hospital Seeing More Babies Born Exposed to Prescription Drugs.” CNN.com. Retrieved from https://www.cnn.com/2012/04/28/health/drug-babies/index.html
Patterson, Eric. “The Effects of Xanax Use.” DrugAbuse.com. Retrieved from https://drugabuse.com/library/the-effects-of-xanax-use/
Raison, Charles (2010, March 23). “Expert Q & A: What Are the Long-Term Brain Effects of Xanax?” CNN.com. Retrieved from http://www.cnn.com/2010/HEALTH/expert.q.a/03/23/xanax.long.term.use.raison/index.html
Raison, Charles (2011, October 4). “Is There a Wrong Way to Detox off Xanax?” CNN.com. Retrieved from http://thechart.blogs.cnn.com/2011/10/04/is-there-a-wrong-way-to-detox-off-xanax/comment-page-1/
Ramirez, Fernando (2017, August 19). “Texas Child Hospitalized After Eating Xanax He Was Told Was a Tic Tac.” Houston Chronicle. Retrieved from https://www.chron.com/news/houston-texas/houston/article/Texas-child-hospitalized-after-eating-Xanax-he-11943500.php
Richards, Chris (2017, April 20). “Soft, Smooth and Steady: How Xanax Turned American Music into Pill-Pop.” The Washington Post. Retrieved from https://www.washingtonpost.com/lifestyle/style/soft-smooth-and-steady-how-xanax-turned-american-music-into-pill-pop/2017/04/19/535a44de-1955-11e7-bcc2-7d1a0973e7b2_story.html?utm_term=.bd5acf4ff0b7
Span, Paula (2018, March 16). “The New Old Age: A Quiet Drug Problem Among the Elderly.” The New York Times. Retrieved from https://www.nytimes.com/2018/03/16/health/elderly-drugs-addiction.html
Substance Abuse and Mental Health Services Administration (2014, December 18). “Combining Benzodiazepines with Other Substances Raises Risks.” Retrieved from https://www.samhsa.gov/newsroom/press-announcements/201412180300
Substance Abuse and Mental Health Services Administration (2014, May 22). “Emergency Departments See Increased Visits Involving the Nonmedical Use of Sedative Alprazolam.” Retrieved from https://www.samhsa.gov/newsroom/press-announcements/201405220400
Substance Abuse and Mental Health Services Administration (2015, October 27). “Types of Commonly Misused or Abused Drugs.” Retrieved from https://www.samhsa.gov/prescription-drug-misuse-abuse/types
Tiefer, Lenore (2015, August 7). “If You Give a Mouse a Xanax.” The Wall Street Journal. Retrieved from https://www.wsj.com/articles/if-you-give-a-mouse-a-xanax-1438978022
U.S. Food and Drug Administration (2016, August 31). “New Safety Measures Announced for Opioid Analgesics, Prescription Opioid Cough Products, and Benzodiazepines.” Retrieved from https://www.fda.gov/drugs/drugsafety/informationbydrugclass/ucm518110.htm.
Weil, Martin (2017, April 25). “Possible Xanax Use at School Investigated in Loudoun.” The Washington Post. Retrieved from https://www.washingtonpost.com/local/possible-xanax-use-at-school-investigated-in-loudoun/2017/04/25/faf25c74-2970-11e7-b605-33413c691853_story.html?utm_term=.ef2a3400f8d5
Williams, Alex (2017, June 10). “Prozac Nation Is Now the United States of Xanax.” The New York Times. Retrieved from https://www.nytimes.com/2017/06/10/style/anxiety-is-the-new-depression-xanax.html
[/expand]