Cocaine Detox Guide
[three-fifths-first]
Leaves of the coca plant, native to Central and South America, release a stimulant and are chewed by rural laborers to keep their energy up. Pure cocaine powder was first extracted in 1860, providing opportunities for more intense stimulation. It is approved for some medical uses, notably local anesthesia, but the majority of users are seeking illegal pleasure or stress relief.
Made into a paste, cocaine is typically snorted or injected. It stimulates the central nervous system to produce and retain more pleasure-enhancing dopamine, resulting in intense, long-lasting euphoria. A crystallized, smokable derivative called “crack” is popular in poorer demographics: crack provides a quicker (though shorter-lived) rush at one-sixth to one-tenth the cost.
[/three-fifths-first]
[two-fifths]
TABLE OF CONTENTS
[/two-fifths][clearfix]
Over 4.7 million Americans abuse cocaine, and over 900,000 have cocaine addiction disorders. About 13 percent of people in addiction treatment name cocaine as their drug of choice. Over a long-term period, ongoing use can result in chronic muscle tremors, psychosis, liver dysfunction and heart failure.
Is cocaine ruining your life? Call: (855) 935-2871
COCAINE WITHDRAWAL SYMPTOMS
Withdrawal from cocaine can be characterized by intense “stress” symptoms:[one-half-first]
- High agitation and difficulty concentrating
- Unusual drowsiness
- Restless sleeping and nightmares
- Depression or anhedonia (loss of pleasure feelings)
- Binge eating
- Tremors
- Body aches or pain spasms
[/one-half-first][one-half]
[/one-half][clearfix]
While cocaine withdrawal rarely causes life-threatening physical symptoms, its mental–emotional effects can drive people to dangerous behavior or even suicide.
Withdrawal duration and intensity can be affected by how long a person has been addicted, the size of regular doses, the setting of the detox attempt, and co-occurring mental disorders such as clinical depression.
- Time to complete withdrawal tends to be directly proportional to time spent addicted.
- People who habitually took larger doses spend more time in withdrawal because their bodies have taken in higher total amounts of cocaine.
- Being exposed to anything that triggered past cocaine use—particularly anything that reminds the patient of related stress factors—is likely to make withdrawal more difficult.
- People who used cocaine to self-medicate depression, or who otherwise struggle with additional mental disorders or drug problems, are at special risk for difficult and prolonged withdrawal.
COCAINE WITHDRAWAL TIMELINE
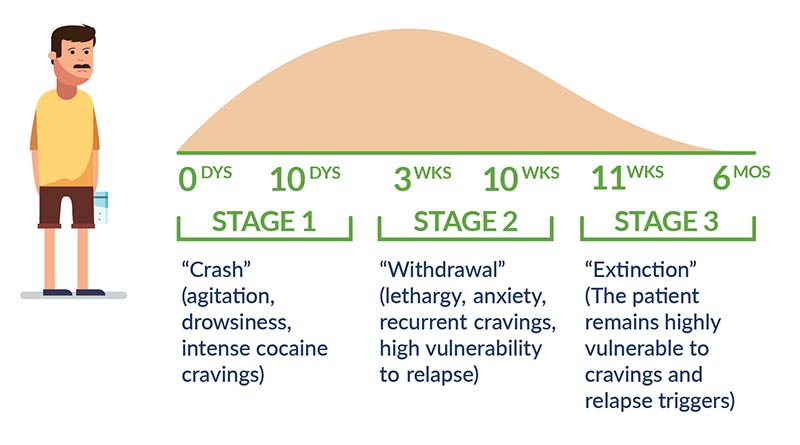
Cocaine is noted for its short half-life: discernible withdrawal symptoms can manifest as soon as 90 minutes after the most recent dose. Unfortunately, perhaps because cocaine exerts particularly strong psychological influence, the time it takes symptoms to disappear completely is often as long as ten days. Many experts consider this only the first phase of withdrawal—the initial “crash”—and propose a three-phase timeline that may last for months:
- 7–10 days of “crash” (agitation, drowsiness, intense cocaine cravings)
- 3–10 weeks of “withdrawal” (lethargy, anxiety, recurrent cravings, high vulnerability to relapse)
- 6 months of “extinction” (the patient remains highly vulnerable to cravings and relapse triggers)
The “crash” period is effectively synonymous with detox, the initial phase of treatment for all chemical addictions. After this stage—which should be undertaken in a hospital with medical supervision—the patient requires additional treatment during “withdrawal” and the early weeks of “extinction.”
INPATIENT TREATMENT FOR COCAINE
For this longer-term treatment, the first important decision is: inpatient or outpatient treatment? Both last up to three months, involve clinical and medical therapy, and cover:
- Diet planning, exercise programs and medical checkups
- Intensive counseling to root out addiction-related problems
- Relapse prevention plans to keep the patient from returning to cocaine
With inpatient, or “residential,” care, the patient stays in medically supervised facilities for up to three months. Inpatient care is highly recommended if:
- The patient has detoxed before (whether at home or in a hospital) and quickly relapsed upon returning to everyday life.
- The patient has any co-occurring mental health disorders that need treatment.
- The patient comes from a family with a history of chemical addictions, mental illness or suicide.
- The patient lacks a strong support network outside the treatment center.
The advantage of inpatient care is that it keeps the patient in a supportive environment with relapse temptations and triggers a safe distance away, and professionally trained staff on hand to tend to emotional or physical needs.
Learn more about Inpatient Drug Rehab
OUTPATIENT TREATMENT FOR COCAINE
With outpatient care, a patient lives offsite and reports to detox facilities for ongoing therapy. Specific approaches vary, from sending clients back to their regular homes and having them return for three-hour appointments three days each week, to providing open housing on the detox center’s campus with lengthy therapy sessions five to seven days a week. Some centers start newly detoxed patients in shorter inpatient programs (up to 35 days) and transition them into outpatient programs.
Outpatient care may be preferable for someone who:
- Is easily stressed by unfamiliar people and settings.
- Is still highly functional in outside responsibilities, and not exposed to cocaine-use triggers in these settings (although it’s important not to make “can’t be away from work too long” the decisive criterion).
- Has supportive family and friends who can be counted on to stay handy and offer ongoing encouragement.
- Will be living close to the best outpatient-treatment option (it’s dangerously easy to let regular attendance lapse when facing out-of-the-way trips at the end of long days).
Learn more about Outpatient Drug Rehab
CAN COCAINE DETOX BE DONE AT HOME?
While outpatient care has advantages after physical detox, the detox itself should always be undertaken in an inpatient setting. Although people have successfully detoxed at home, it’s a serious risk, especially for anyone who has co-occurring depression issues or has previously considered or attempted suicide.
Even in the best-case scenario—a person has used cocaine for a relatively short time, is in overall good health and has access to trustworthy support—medically supervised inpatient treatment is preferable because:
- A detox center has the facilities to make patients as comfortable as possible.
- Certified detox counselors are best qualified to prepare patients for dealing with symptoms.
- Detox staff are well trained in recognizing and defusing medical dangers.
- Detox staff have seen most symptoms before, and are in the best position to reassure the patient that the negative effects are common and won’t last forever.
Detox centers also have access to licensed M.D.s who can recommend higher-tech treatment approaches, including prescription medications. This is a less likely scenario with cocaine than with substances where withdrawal manifests intense physical symptoms, and currently there are no FDA-approved medications for treating cocaine addiction. However, some medications show potential to reduce intensity of withdrawal symptoms and risk of relapse:
- Disulfiram, frequently used in alcoholism treatment, also reduces cocaine cravings in many people.
- Buprenorphine and naltrexone, both long approved for opioid addiction treatment, are being tested for cocaine detox.
- Propranolol, a beta blocker commonly prescribed for hypertension and anxiety, might help reduce paranoia and suicidal thoughts.
- Other antidepressants and antianxiety medications, considered on a case-by-case basis, can reduce the intensity of more dangerous symptoms and perhaps shorten the withdrawal period.
- A “cocaine vaccine” is being tested for its potential in reducing relapse.
TAPERED VS. COLD TURKEY
With some substances (particularly benzodiazepines and methadone), detox providers frequently use the “tapered” approach, administering gradually reduced doses of the addictive substance rather than abruptly cutting off the supply. Most often recommended for people at risk for severe withdrawal symptoms, “tapering” can spare the body and brain some “cold turkey” shock. It is rarely used with cocaine addiction.
CONSIDERATIONS/HOW TO DECIDE WHAT IS RIGHT FOR YOU
Besides inpatient/outpatient options and medical treatment approaches, factors to consider in choosing a treatment program include:
- Location (geographically convenient is usually best)
- Philosophical approach
- Reputation and community involvement
- Experience treating cocaine addiction specifically
Depending on treatment methods, additional facilities provided and individual patient needs, cocaine detox and rehab can be expensive. Fortunately, most health insurance policies, including Veterans Affairs, cover at least part of addiction-treatment expenses. Some healthcare costs are even tax deductible.
RECOVERY SUCCESS AND AFTERCARE SERVICES FOR COCAINE

These techniques include ongoing therapy, treatment for co-occurring illnesses, and support-group attendance. (Over 80 percent of support-group participants report that empathy and accountability reduce relapse temptations.) Other elements of effective aftercare include:
- Drug testing
- Social events
- Quick help in case of intense temptation or actual relapse
Learn more about Cocaine Aftercare
Is cocaine ruining your life? Get help now
[expand title=" Sources:" targclass="highlight"]
Australian Government Department of Health (2004, April). “The Cocaine Withdrawal Syndrome.” Retrieved from http://www.health.gov.au/internet/publications/publishing.nsf/Content/drugtreat-pubs-modpsy-toc~drugtreat-pubs-modpsy-3~drugtreat-pubs-modpsy-3-7~drugtreat-pubs-modpsy-3-7-cws
National Institute on Drug Abuse (2016, May). “Cocaine: How Is Cocaine Addiction Treated?” Retrieved from https://www.drugabuse.gov/publications/research-reports/cocaine/what-treatments-are-effective-cocaine-abusers
National Institute on Drug Abuse (2016, May). “What Are the Long-Term Effects of Cocaine Use?” Retrieved from https://www.drugabuse.gov/publications/research-reports/cocaine/what-are-long-term-effects-cocaine-use
National Institute on Drug Abuse (2016, June). “What Is Cocaine?” Retrieved from https://www.drugabuse.gov/publications/drugfacts/cocaine
Tracy, Kathlene, and Samantha P. Wallace (2016, September 29). “Benefits of Peer Support Groups in the Treatment of Addiction.” Substance Abuse and Rehabilitation (2016, No. 7, pp. 143–154). Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5047716/
[/expand]